
Co-sourcing – The best revenue cycle management solution for you
Reform initiatives have changed the complexion of the healthcare industry. Hospitals and medical groups are facing increased pressure to lower their cost base and inject more revenue into their organization. The one area where most hospitals have engaged in innovation is the revenue cycle.
The revenue cycle is a critical building block on which all transformation efforts rest. The relationship between revenue cycle vendors and hospitals has changed from a mere contractual relationship to a long-term partnership that will help them transition towards new payment models, experiment with revenue cycle tools, and meet compliance demands.
But there is one piece of the puzzle that is forever missing. Transparency. Transparency is the cornerstone of any long-term partnership but most healthcare organizations don’t have a clear window into their revenue cycle operations.
According to a survey by HIMSS analytics, 69% of healthcare organizations surveyed revealed that they used multiple vendor solutions to manage their revenue cycle. This laundry list of systems adds to operational costs and makes monitoring the revenue cycle a nightmare.
1. Project management system:
Things can get pretty awry if there’s no streamlined system to track the progress of revenue cycle processes and the performance metrics of teams. A project management system should offer clear insights into the everyday progress of tasks and allow users to schedule and monitor tasks.
A revenue cycle vendor that offers a project management system enables healthcare organizations to make course corrections and manage shifts in payer mixes and reimbursement models without losing sight of the big picture.
Here is a snapshot of BillingParadise’s project management system built and customized to track our clients’ Revenue Performance at one place.

2. Communication management system:
Communicating with revenue cycle vendors can be grueling without a communication system that quickens query management and makes raising and resolving tickets easy. Communication is the magic glue that binds disparate business office operations and having a communication system in place, or insisting on one right at the outset, minimizes the risk of miscommunication and lost tickets.
Query and ticketing
Remote billers find it next to impossible to coordinate with In-house staff. In-house billers and coders are worked off their feet and emailing or calling the remote billing office adds to their massive to-do list. A query and ticketing management system resolves this awning gap between in-house billers and offsite staff.
Multiple tabs are a pain
Yes. Anybody who’s had the misfortune of working with multiple systems and tabs knows they are a time suck. One secure communication system enables people from different departments and locations to work together without losing the common thread.
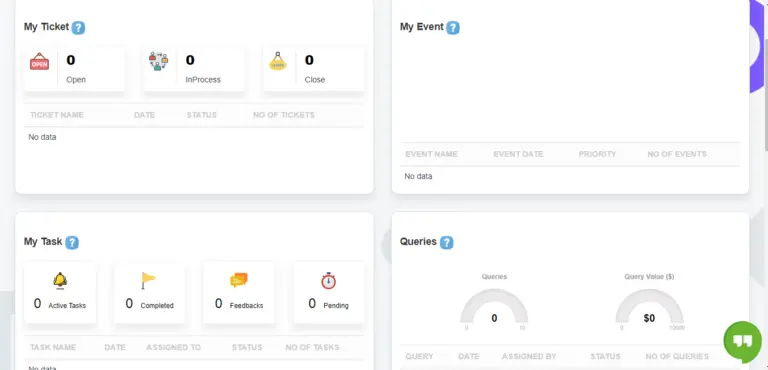
How BillingParadise deals with its clients through this all one in communication platform.
If you are thinking about hiring a third party RCM vendor then this checklist is built for you
3. Credentialing and contract renewal:
If your providers are being denied on out-of-network claims or are seeing reductions in benefits because they are considered nonparticipating, it’s an indication of credentialing issues, says Penny Noyes, CHC, MGMA member, president, Health Business Navigators, Bowling Green, Ky.
If a provider is participating with a particular payer or product due to credentialing issues, make sure front-desk staff know not to schedule patients with those payers or products until the issue is fixed to avoid additional denials. “The front office is a key part of the information chain that is often forgotten about,” Noyes says. If your practice has more than 10 providers, you probably want to consider using credentialing software to assist with your tracking and workflow, Noyes added. Source MGMA.
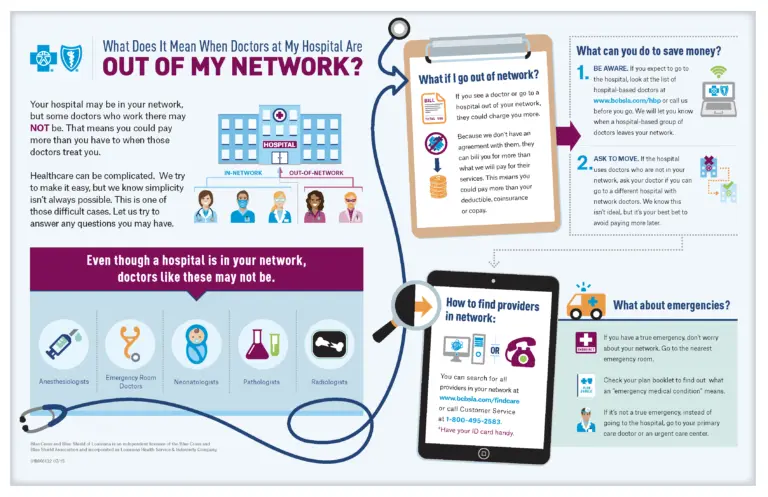
Credentialing new providers and managing re-credentialing tasks takes up a lot of time. And if a revenue cycle vendor doesn’t offer an integrated solution, takes up a lot of time and hard disk space as well. A credentialing solution that automatically generates notifications on outdated/missing information and centralized operations quickens and speeds up the credentialing process. A contract management system minimizes the work burden placed on staff to handle and negotiate managed care contracts. A contract management software helps hospitals to spot and analyze payment variances right down to the service line level.
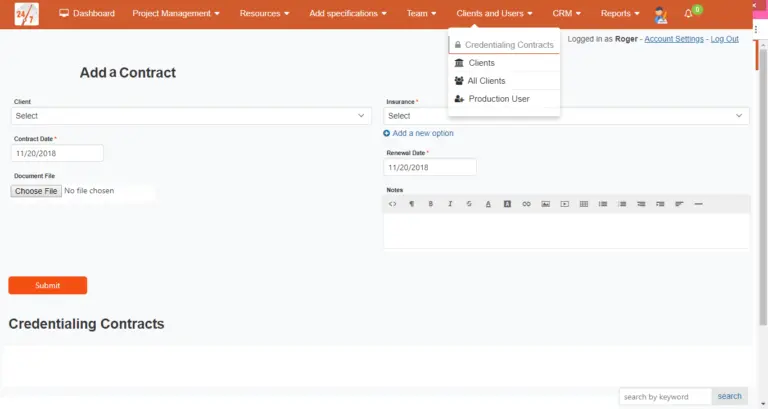
To avoid installing and working with a credentialing and contract management software a solution that is built into the RCM solutions provided by vendors eliminates unnecessary costs and the tedium of working with a laundry list of systems.
Know how BillingParadise helped an Ob-Gyn centre increase revenue by adding out-of-network patients.
Monitoring contract specifics is tedious especially when there are multiple payers and providers involved. Implementing a system or tickler that sends an alert every time a contract expires helps in managing contracts and alerting providers of expiring contracts and renewals. Except for federal contracts, there is room for negotiation in most contracts. A contract management system can put offsite and in-house revenue cycle teams on the same page and help in building stronger contracts.
4. Denial Management Platform:
Around two-thirds of denials are recoverable and 90% of denials are preventable. Look for a vendor who offers a denial prevention and reporting system. Over half of the respondents surveyed by RACMonitor recently reported paying more than $30 per account to resolve denials, with 38 percent paying more than $40. This points to an industry-wide opportunity to seek out and implement systems that will reduce this cost.

Reform initiatives have changed the complexion of the healthcare industry. Hospitals and medical groups are facing increased pressure to lower their cost base and inject more revenue into their organization. The one area where most hospitals have engaged in innovation is the revenue cycle.
The revenue cycle is a critical building block on which all transformation efforts rest. The relationship between revenue cycle vendors and hospitals has changed from a mere contractual relationship to a long-term partnership that will help them transition towards new payment models, experiment with revenue cycle tools and meet compliance demands.
But there is one piece of the puzzle that is forever missing. Transparency. Transparency is the cornerstone of any long term partnership but most healthcare organizations don’t have a clear window into their revenue cycle operations.
According to a survey by HIMSS analytics, 69% of healthcare organizations surveyed revealed that they used multiple vendor solutions to manage their revenue cycle. This laundry list of systems adds to operational costs and makes monitoring the revenue cycle a nightmare.

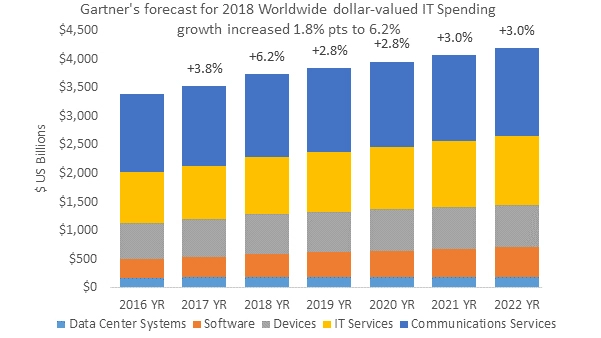
Cost of IT spending
To effectively contain costs and gain more transparency into operations it is imperative that hospitals partner with revenue cycle vendors who offer an integrated RCM solution that eliminates the need for multiple vendor systems. A culture of accountability has to be fostered to gain insights into the many moving parts of the revenue cycle structure.
What to look for while partnering with a revenue cycle management vendor?
To avoid the additional costs and headache of working with multiple systems hospitals must work with a revenue cycle vendor who offers a comprehensive set of revenue cycle and change management tools that offer enhanced reporting capabilities and big-picture insights.
1. Project management system:
Things can get pretty awry if there’s no streamlined system to track the progress of revenue cycle processes and the performance metrics of teams. A project management system should offer clear insights into the everyday progress of tasks and allow users to schedule and monitor tasks.
A revenue cycle vendor who offers a project management system enables healthcare organizations to make course corrections and manage shifts in payer mixes and reimbursement models without losing sight of the big picture.
Here is a snapshot of BillingParadise’s project management system built and customized to track our clients’ Revenue Performance at one place.
2. Communication management system:
Communicating with revenue cycle vendors can be gruelling without a communication system that quickens query management and makes raising and resolving tickets easy. Communication is the magic glue that binds disparate business office operations and having a communication system in place, or insisting on one right at the outset, minimizes the risk of miscommunication and lost tickets.
Query and ticketing
Remote billers find it next to impossible to coordinate with In-house staff. In-house billers and coders are worked off their feet and emailing or calling the remote billing office adds to their massive to-do list. A query and ticketing management system resolves this awning gap between in-house billers and offsite staff.
Multiple tabs are a pain
Yes. Anybody who’s had the misfortune of working with multiple systems and tabs knows they are a time suck. One secure communication system enables people from different departments and locations to work together without losing the common thread.
How BillingParadise deals with its clients through this all one in communication platform.
If you are thinking about hiring a third party RCM vendor then this checklist is built for you
3. Credentialing and contract renewal:
If your providers are being denied on out-of-network claims or are seeing reductions in benefits because they are considered nonparticipating, it’s an indication of credentialing issues, says Penny Noyes, CHC, MGMA member, president, Health Business Navigators, Bowling Green, Ky.
If a provider is nonparticipating with a particular payer or product due to credentialing issues, make sure front-desk staff know not to schedule patients with those payers or products until the issue is fixed to avoid additional denials. “The front office is a key part of the information chain that is often forgotten about,” Noyes says. If your practice has more than 10 providers, you probably want to consider using credentialing software to assist with your tracking and workflow, Noyes added. Source MGMA

Credentialing Renewals
Credentialing new providers and managing re-credentialing tasks takes up a lot of time. And if a revenue cycle vendor doesn’t offer an integrated solution, takes up a lot of time and hard disk space as well. A credentialing solution that automatically generates notifications on outdated/missing information and centralized operations quickens and speeds up the credentialing process. A contract management system minimizes the work burden placed on staff to handle and negotiate managed care contracts. A contract management software helps hospitals to spot and analyze payment variances right down to the service line level.

Simple yet effective credentialing contract renewal management system built by BillingParadise
To avoid installing and working with a credentialing and contract management software a solution that is built into the RCM solutions provided by vendors eliminates unnecessary costs and the tedium of working with a laundry list of systems.
Know how BillingParadise helped an Ob-Gyn centre increase revenue by adding out-of-network patients.
Monitoring contract specifics is tedious especially when there are multiple payers and providers involved. Implementing a system or tickler that sends an alert every time a contract expires helps in managing contracts and alerting providers of expiring contracts and renewals. Except for federal contracts, there is room for negotiation in most contracts. A contract management system can put offsite and in-house revenue cycle teams on the same page and help in building stronger contracts.
4. Denial Management Platform:
Around two-thirds of denials are recoverable and 90% of denials are preventable. Look for a vendor who offers a denial prevention and reporting system. Over half of the respondents surveyed by RACMonitor recently reported paying more than $30 per account to resolve denials, with 38 percent paying more than $40. This points to an industry-wide opportunity to seek out and implement systems that will reduce this cost.

An effective denial management system should track, classify and identify denial patterns.
The denial management of your RCM vendor should
- Classify denial codes into different groupings for easy follow-up
- Provide user-defined queues
- Assign tasks to variance teams automatically
- Identify denial patterns
- Interface with your EHR easily
Have a look at the hospital denial management best practices here
A denial management system that benchmarks denials against MGMA standards optimizes denial operations and ensures you’re in line with industry best practices.
5. AR Management platform:
The recent rise in High-Deductible Health Plans (HDHP) and, consequently, patient payment responsibilities have compounded the challenge of liquidating AR and tightening AR management processes. Tracking key performance reports helps healthcare organizations to identify outliers, optimize revenue capture and spot overlooked pockets of revenue in your AR portfolio.

Common features of a hospital AR management software
Granular reports that offer multi-level drill downs are the need of the hour. In-depth reports highlight key risk segments, streamline AR follow-up activities and improve relationships with payers and patients. It will also throw light on the major drivers behind AR trends.
6. Revenue Analysis Platform:
The post-reform healthcare environment throws up new challenges every day. And the biggest challenge hospitals face is tracking and analyzing vital financial data. Study after study emphasizes on the importance of data mining and making workflow improvements. The slant is on revenue cycle efficiency, compliance, and more updated RCM processes.
Without extracting, identifying and analyzing financial data it is going to be extremely tough to keep pace with the changes and plan for the future.
It is important that healthcare organizations receive reports such as:
- Claim rejection info
- Denial percentage
- The average life of denials
- Percentage of no-response claims
- Insurance payment details
- Patient payment information.
- The time between DOS and billing date
- Claim volume
- Claim lags
- And daily collection activities.
A revenue cycle partner who is truly invested in the long term financial stability of healthcare organizations needs to offer a system that makes receiving vital revenue cycle reports in real time a possibility.
7. Service Level Agreement compliance :
Outsourcing needn’t mean releasing control. With strong and uncomplicated SLAs in place, healthcare organizations can ensure they steer their revenue cycle in the right direction. It is important that there is a vendor management function in place as a part of externalizing initiatives.
Hospitals who sign service level agreements that are foolproof can be assured of year-over-year improvement in yield. To drive movement towards best practice using HFMA MAP keys to compare performance and set targets against industry standards is suggested.
A few objective metrics that every SLA must contain:
-
- AR benchmarking with HFMA standards
- Denial reports
- Claim rejection reports (<%)
- Eligibility verification (prior 24 hrs of visiting patients)
- Coding Reviews
Here is a glimpse of how SLAs set at BillingParadise help resolve key issues

Performance tracking through a single window by comparing real-time data with industry benchmarks.

Reviewing the performance metrics of the team to ensure high performance
All in one platform for monitoring a healthcare organization’s revenue performance.


