Revenue cycle management in 2026 is not what it was even three years ago. Denial rates hover between 11 and 12 percent nationally. Days in A/R routinely stretch past 50. Billing staff turnover runs between 30 and 40 percent. The global healthcare RCM outsourcing market, hitting $23.7 billion in 2022 and racing toward $62.4 billion by 2028 at a 17.4 percent CAGR according to IMARC Group, has flooded the landscape with more vendor noise than any evaluation process was designed to filter.
Every vendor now claims AI. But not every organization needs it in the same way, or at all. For midsized or large healthcare organizations above $10 million in annual revenue, a two-point swing in net collection rate means $200,000 to $500,000 gained or lost.
The question worth asking before any vendor conversation is not just “how good is their AI?” It is whether an AI-powered RCM is genuinely the right fit for your organization right now, and what you give up, or gain, by choosing either path.
This guide was built so you can make that distinction clearly. We cover the evaluation criteria that separate vendors who deliver from those who only demo well, and at every major decision point, we lay out what the AI-powered and traditional approaches each bring to the table, so you can judge for yourself.
Looking for an RCM Partner That Delivers Measurable Results?
Connect with Our Team to Discuss Your Revenue Cycle Goals and Performance Targets
Factors Influencing RCM Outsourcing in 2026: How Traditional & AI-enabled RCM Services Support
Managing the financial aspects of patient care has become an increased challenge in today’s healthcare landscape, and the providers feeling that pressure most acutely are increasingly choosing to act.
According to the HFMA, 95 percent of health systems plan to purchase RCM or finance technology, a clear signal that the need for more sophisticated, integrated, and scalable revenue cycle support is no longer a future consideration. It is a present one.
 Organizations are not just looking to fix problems. They are looking to build resilience, grow with confidence, and operate with greater financial clarity. Whether the right path runs through a traditional or AI-powered RCM partner depends on where each organization’s specific gaps live.
Organizations are not just looking to fix problems. They are looking to build resilience, grow with confidence, and operate with greater financial clarity. Whether the right path runs through a traditional or AI-powered RCM partner depends on where each organization’s specific gaps live.
Here is what is driving that evaluation.
To Manage Rising Costs and Improve Financial Efficiency
The average cost to collect runs between 3 and 7 percent of net patient revenue, up to $1.4 million annually for a $20 million organization. Maintaining an in-house RCM department requires significant investment in personnel, training, technology infrastructure, and software licensing.
On average, healthcare organizations see cost savings of 20 to 40 percent when they transition from an in-house RCM department to outsourced solutions, driven by reduced staffing costs, eliminated training expenses, and removed software overhead.
Traditional RCM partners convert those fixed internal costs into a more predictable outsourced model.
AI-powered partners go further by reducing the labor embedded in repetitive tasks through intelligent automation. McKinsey estimates this could lower RCM operating costs by 30 to 60 percent over time.
The right question is not which model is cost-effective, but which model produces a lower, more sustainable cost-to-collect relative to your claim volume and operational complexity.
To Improve Revenue Performance and Cash Flow
Consistent cash flow is the central priority of any RCM investment, yet the system consistently works against it.
According to Experian Health’s State Of Claims Report, up to 30 percent of denied claims are never reworked, representing permanent, unrecoverable revenue loss.
Traditional RCM vendors recover revenue through disciplined billing workflows and experienced payer follow-up.
AI-powered vendors pursue revenue optimization through prevention, denial scoring before submission, pricing automation, and contract monitoring that surfaces underpayments at scale before they become write-offs.
Key Performance Metrics (AI Vs Traditional RCM)
| Metric | Traditional RCM | AI Powered RCM |
|---|---|---|
| Denial Rate | 15–20% | 5–8% |
| Days in AR | 50–65 days | 25–35 days |
| Clean Claim Rate | 75–85% | 95–98% |
| Cost to Collect | 3–5% | 1–2% |
To Manage Growing Operational Complexity
While coding and billing practices are generally consistent across modalities, each specialty can have unique requirements and documentation, and RCM solutions must accommodate these various requirements to be effective.
CMS added over 500 new ICD-10 codes in 2024 alone. Payer rules shift continuously without advance notice. For multi-specialty organizations, the volume of payer-specialty rule combinations exceeds what any in-house team can reliably track.
Experienced RCM teams must stay current on all regulatory requirements, such as the latest coding updates and regulatory changes to HIPAA, to ensure accurate claims submissions and minimize denials.
Traditional partners absorb that complexity through domain expertise and structured workflows. AI-powered partners adapt continuously, detecting payer behavior shifts in real-time denial data before billing teams have been formally notified, a critical advantage as organizational complexity grows.
To Address Staffing Shortages and Reduce Administrative Burden
Researchers forecast nationwide labor shortages across most healthcare occupations over the next 15 or more years, and these employment gaps are especially troublesome for specialty providers who often operate with smaller teams and fewer locations to attract and retain skilled staff.
In the revenue cycle management industry, worker turnover rates are very high, with more than 30 percent of billing and coding positions turning over every year, creating constant retraining costs and performance gaps.
Traditional RCM outsourcing removes the burden of recruiting, training, and managing a billing department entirely.
AI-powered RCM reduces the structural reliance on headcount by automating the tasks that consume the most labor per claim, such as eligibility checks, payment posting, and claim scrubbing, so existing staff can focus on escalations and judgment-intensive work.
Professional RCM companies have established training programs, career pathways, and competitive pay structures that maintain staff stability and experience, providing consistency that in-house teams under turnover pressure rarely sustain.
To Improve Efficiency Through Automation and Intelligent Workflows
As claim volumes grow and staff capacity stays constrained, manual workflows become a bottleneck at every stage. Seamless integration with a practice’s existing EHR and practice management systems is fundamental to choosing a service provider. Because, efficiency gains from automation are only possible when data flows cleanly between systems without manual intervention.
Traditional models address efficiency through process standardization and outsourced team capacity.
AI-powered models introduce RCM automation across patient intake, eligibility verification, prior authorization tracking, payment posting, and AR queue prioritization, repositioning experienced billing staff from repetitive execution toward the decisions that genuinely move revenue.
To Handle a Complex and Evolving Payer Mix
As health plans, regulations, and payer rules continue to complicate the market, practices must keep up with the changes and update their processes and technology to maintain steady cash flow.
With a continuing shortage of skilled RCM staff, a complex payer mix creates a compelling case for a skilled RCM partner to oversee the payer relationship.
Medicare Advantage now covers more than half of all Medicare beneficiaries, with authorization denial rates significantly higher than traditional fee-for-service.
Traditional RCM partners apply relationship-based payer expertise, knowing which payers require peer-to-peer reviews and where escalation paths exist.
AI-powered partners analyze historical payer behavior dynamically, optimizing submission strategy at a scale and consistency that experience-based approaches cannot match alone.
To Reduce Claim Denials and Protect Margins
According to a KFF consumer survey, insurers of qualified health plans (QHPs) sold on HealthCare.gov denied 19% of in-network claims in 2024 and 37% of out-of-network claims for a combined average of 20% of all claims, all similar to 2023, often traced to poor preauthorization requirements or coding and documentation errors.
Denied inpatient and outpatient claim amounts rose 12% and 14% respectively from 2024 to 2025. Denials tied to medical necessity rose 70 percent in dollar value, reaching $450 per denial on average.
Traditional vendors address denials through experienced appeal specialists with deep payer knowledge, achieving strong overturn rates on reworked claims.
AI-powered vendors shift the model from recovery to prevention, predictive denial scoring flags at-risk claims before submission, with mature platforms achieving clean claim rates of 97 to 98 percent against a national average hovering near 85 percent.
To Access Technology Your Organization Cannot Realistically Build In-House
The high cost of replacing technology, particularly an aging practice management system that may or may not be integrated with other clinical and administrative software applications, can be a significant financial burden for healthcare practices.
But with the rise in cyberattacks and the growing complexity of payer rules and regulations, maintaining updated, integrated technology is no longer optional.
Traditional partners provide access to proven systems without requiring capital investment.
AI-powered partners provide access to predictive analytics, intelligent automation, and real-time AI dashboards that would take years and significant data science resources to build independently.
To Improve Visibility and Enable Smarter Financial Decisions
Leadership teams need to know where revenue is delayed, which payers are underperforming, and what cash flow looks like next quarter, not last month.
Data-driven insights empower informed decisions, and the right RCM provider should offer robust analytics dashboards providing real-time visibility into key performance metrics like medical coding accuracy, claim denials, and patient collection rates.
With outsourced RCM, healthcare providers can get detailed reports on important performance parameters like clean claim rates, denial rates, collection ratios, and payer performance measures, enabling data-driven decisions and identifying ways to improve processes.
Traditional vendors deliver this through periodic reporting and experienced analyst interpretation. AI-powered vendors surface it continuously through real-time AI dashboards and revenue forecasting, by the time a trend appears in a monthly report, it has typically been running for weeks.
To Enhance the Patient Financial Experience
Revenue cycle performance and patient experience are more connected than most organizations account for. Billing confusion, unexpected balances, and poor payment communication are among the leading causes of patient dissatisfaction and delayed collections.
Traditional vendors address patient financial experience through dedicated patient collections teams and financial counseling workflows.
AI-powered vendors enhance patient intake with digital tools that estimate financial responsibility upfront, automate payment plan communications, and reduce the manual burden on front desk staff, which drives so much of the patient billing friction.
To Support Growth, Scalability, and Practice Independence
Multiple facility sites may require recruiting physicians, other clinical staff, and both financial and administrative support across different geographic locations, which may have different rules and regulations for credentialing and billing. As a practice expands into more markets, a scalable staffing model becomes critical to managing administrative costs in the revenue cycle.
The 2024 Physician Practice Benchmark Survey shows that private physician practices now account for less than half of US physicians in most specialties, with the shift often driven by inadequate payment rates, increasing operating costs, and burdensome regulatory requirements.
To Strengthen Compliance and Reduce Regulatory Exposure
The ever-changing regulatory requirements in healthcare, from HIPAA privacy rules to changing billing codes and compliance standards, shift the major compliance burden onto specialized firms that have made it their business to keep abreast of all relevant regulations.
OIG enforcement activity is increasing. Medicare Advantage audits are expanding. The HHS Office for Civil Rights fined Green Ridge Behavioral Health $40,000 following a ransomware attack affecting 14,000 patient records.
A professional medical billing services company will utilize advanced security protocols and undergo regular audits to ensure the highest level of patient information protection.
Traditional partners manage compliance through certified coders, structured documentation standards, and periodic internal reviews.
AI-powered partners embed it continuously, with automated audit trails, real-time coding validation, and anomaly detection before claims are filed. For AI-powered vendors, governance matters equally: model decisions need to be explainable, auditable, and monitored for drift as algorithms evolve.
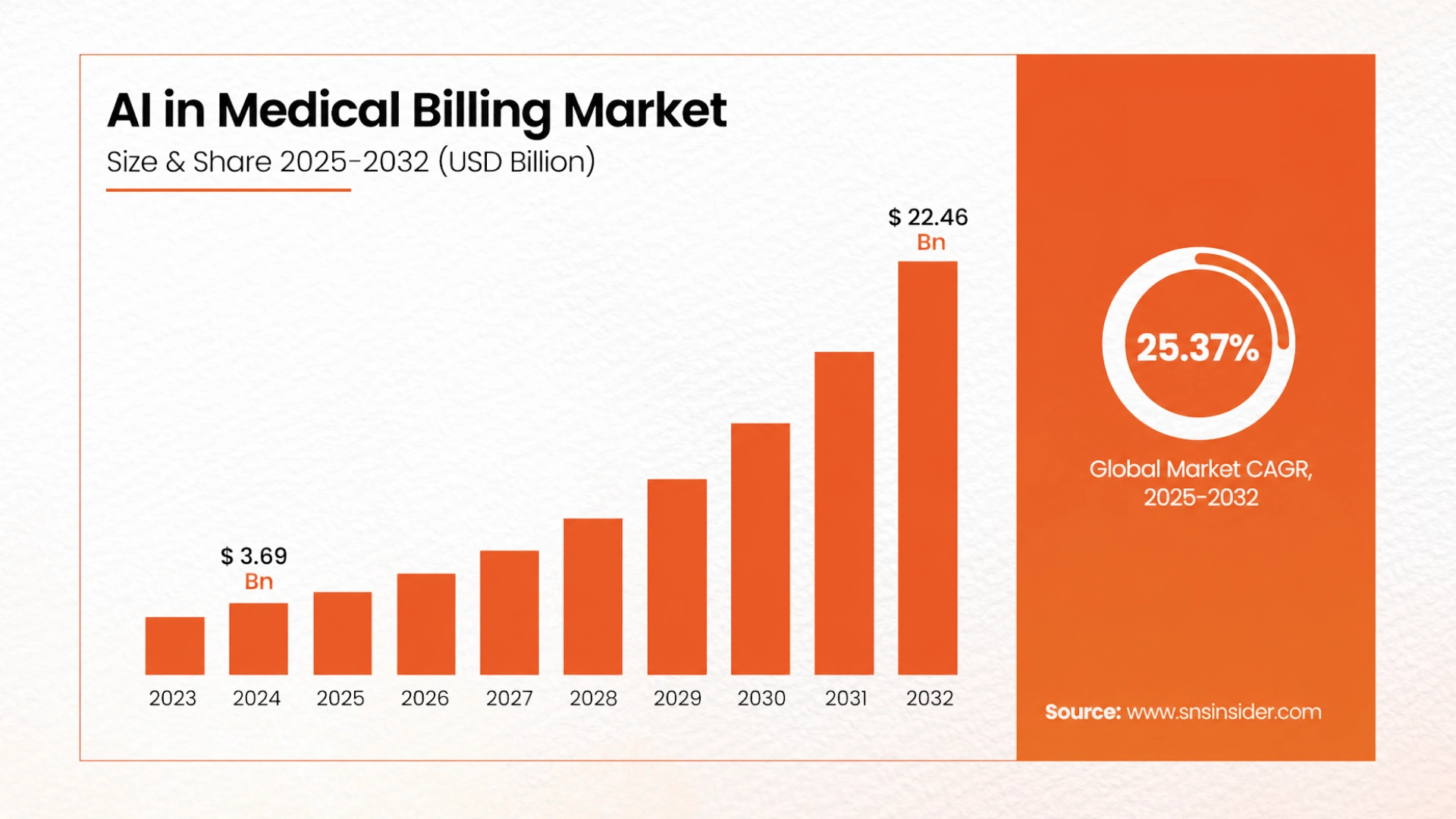
The AI in the Medical Billing Market was valued at USD 3.69 billion in 2024 and is expected to reach USD 22.46 billion by 2032, growing at a CAGR of 25.37 percent. McKinsey estimates AI could reduce RCM costs by 30 to 60 percent while accelerating collections and freeing staff for higher-value work.
And Sometimes, Because the Current Vendor Is No Longer Delivering
A common and often underacknowledged driver of RCM vendor evaluation is straightforward: the current partner has stopped performing. Stagnant collections. Denial rates that have not moved in multiple quarters. Reporting that shows what happened but not why. Account teams that respond to problems rather than getting ahead of them.
Our Jan. 6, 2026, MGMA Stat poll found the biggest revenue cycle leaks for practices today are denials and appeals (48%), followed by front end issues (23%), billing/collections (14%), coding (13%), and charge posting (2%). The poll had 288 applicable responses.

Hospitals spent $43 billion in 2025 trying to collect payments insurers already owed. Bad debt was up 10 percent.
When underperformance is the trigger, the evaluation question is specific:
Does the organization need a more reliable traditional partner who delivers consistently on what was promised, or a more capable AI-powered partner whose capabilities address problems the previous vendor’s model was never designed to solve?
The answer depends on an honest diagnosis of what failed, not just a desire for something different.
Detailed Feature Comparison – Traditional RCM Vs AI-Powered RCM
| Area | Traditional RCM | AI-Powered RCM |
|---|---|---|
| Coding & Billing |
Manual coders review notes; error-prone and slow
Higher error rate |
NLP auto-suggests ICD/CPT codes from clinical notes
95%+ accuracy |
| Prior Authorization |
Phone/fax-heavy process; 2–5 day turnaround
Delays common |
AI auto-submits, tracks, and follows up in real time
Hours instead of days |
| Denial Management |
Reactive denial handling after claim rejection
Revenue leakage risk |
Predictive AI flags denial risks before submission
Prevention-first approach |
| Eligibility Verification |
Manual verification at check-in; missed errors
Delays & write-offs |
Automated real-time eligibility checks across payers
Instant & accurate |
| Patient Collections |
Generic payment plans and paper statements
Low collection rate |
Propensity-to-pay scoring with personalized outreach
Higher yield |
| Reporting & Analytics |
Retrospective dashboards and manual reporting
Always looking back |
Predictive analytics with real-time alerts
Forward-looking insights |
| Scalability |
Scales by adding headcount and operational cost
Expensive to scale |
Scales through automation with minimal cost increase
Cost-efficient |
| Staff Role | Primarily transactional work like data entry and follow-ups | Focus shifts to oversight, exception handling, and complex cases |
| Implementation |
Quick setup with lower upfront cost
Low barrier to entry |
Requires integration and change management
Longer ramp-up |
Key Vendor Evaluation Criteria To Choose An RCM Partner
RCM Domain Expertise and Healthcare Specialization
Strong partners, AI-powered or traditional, have deep healthcare revenue cycle experience across multiple specialties, payer types, and regulatory environments. Their teams include certified coders, denial specialists, compliance experts, and operational leaders who understand how policy changes translate into everyday billing risk.
Where traditional RCM Vendor excels?
Years of relationship-based payer knowledge, complex appeals judgment, and specialty-specific coding nuance are hard to replicate through automation alone. If your denial mix skews toward medical necessity appeals or clinical documentation disputes, human expertise remains the sharper tool.
Where AI-powered Vendor excels?
Pattern recognition across millions of claims surfaces denial trends faster than any individual analyst can. A platform that has processed thousands of claims from your specific payer combination can surface risks a human reviewer would not catch until the denial has already landed.
Note: During evaluation, ask vendors how their teams, or their models, handled a specific payer policy change in the past twelve months. The quality of that answer tells you more than any feature list.
End-to-End Revenue Cycle Coverage
Fragmentation, accountability gaps between front-end, mid-cycle, and back-end functions, is one of the most persistent causes of that kind of revenue loss.
Where traditional RCM Vendor excels?
Experienced firms with long-tenured billing specialists often have strong ownership across the full cycle, particularly in high-touch denial management and payer follow-up. Accountability is person-driven and visible.
Where AI-powered Vendor excels?
Unified platforms can connect eligibility data, claim history, coding patterns, and denial outcomes in ways that siloed human teams rarely achieve. When the same system processes a claim from scheduling through final settlement, pattern detection improves at every stage.
Note: Regardless of model, fragmented coverage is a red flag. Verify that your shortlisted vendors own the full cycle, not just the stages where they excel in their pitch.
Revenue Performance Optimization
Revenue performance is the ultimate measure of RCM effectiveness, not activity metrics or operational outputs, but the actual dollars captured from covered services. Both models pursue this goal, but through meaningfully different mechanisms that produce different risk and reward profiles at different points in the revenue cycle.
Where traditional RCM Vendor excels?
Established workflows and institutional knowledge of payer behavior translate into reliable, consistent collection performance. When complex underpayments or aged accounts require persistent human follow-up, experienced billing teams often outperform automated platforms on recovery rates.
Where AI-powered Vendor excels?
Predictive insights identify revenue leakage before it materializes, flagging claims likely to be underpaid, denied, or delayed before submission. This upstream pressure on reimbursement outcomes reduces the volume of revenue that ever requires recovery in the first place.
Note: Ask vendors to break down their revenue performance metrics between prevention and recovery. A platform that prevents denials will show different numbers than one that excels at appealing them, and your existing denial mix should determine which profile you need more.
Operational Efficiency Model
How work gets done inside an RCM operation matters as much as what gets done. Operational efficiency determines the cost structure, scalability, and ceiling performance of any revenue cycle function, and the two models approach it from fundamentally different directions.
Where traditional RCM Vendor excels?
Staff-driven execution, when supported by standardized processes and experienced team leads, produces consistent, repeatable performance. Accountability is visible, escalation paths are clear, and complex judgment calls can be routed to the right person quickly.
Where AI-powered Vendor excels?
Intelligent work allocation reduces manual effort and improves throughput without proportional headcount increases. Automation handles high-volume, low-complexity tasks, eligibility verification, payment posting, work queue prioritization, freeing staff for the exceptions that require human judgment.
Note: Ask vendors where manual intervention still occurs in their workflow and why. The answer reveals where their efficiency model has real limits and where your team would be absorbing work they are not accounting for in their pitch.
Risk, Denial and Compliance Management
Denial management is where revenue cycle failures become most visible, but by the time a denial lands, the underlying failure has usually already occurred upstream. How a vendor approaches risk at the front end of the cycle is as important as how they recover from it at the back end.
Where traditional RCM Vendor excels:
Resolution-based workflows for denial management are well-established in experienced RCM firms. Complex appeals requiring clinical documentation, medical necessity arguments, or payer-specific escalation paths benefit from the judgment and relationship capital that tenure provides.
Where AI-powered Vendor excels:
Continuous analytics monitoring identifies claim-level risk before submission, catching documentation gaps, coding inconsistencies, and payer-specific triggers that are predictive of denial. Proactive intervention at the pre-submission stage reduces denial volume rather than just managing it after the fact.
Note: Ask vendors for their denial prevention rate, not just their appeal success rate. Prevention and recovery are different capabilities, and the most expensive denial is always the one that requires the most effort to resolve.
AI Capabilities and Automation Maturity
This criterion looks different depending on which model you are evaluating.
Where traditional RCM Vendor excels?
Many experienced traditional firms have integrated automation into eligibility checks, payment posting, and work queue prioritization without positioning themselves as AI companies. That can be entirely adequate depending on your needs. The question is whether intelligent automation is available at the workflow level, not necessarily at the platform level.
Where AI-powered Vendor excels?
AI embedded throughout the cycle, not layered on top as a feature, enables continuous learning from your specific claims history rather than relying on static rules. The platform should perform meaningfully differently today than it did twelve months ago, with operational data to support that claim.
Note: Ask AI-powered vendors specifically: how does your platform perform differently today than it did twelve months ago, and what drove that change? Vendors that cannot answer that question with operational specificity are selling marketing language, not maturity. What matters most is not the AI label, it is whether the technology actively prevents denials rather than just documenting them.
Visibility and Decision Support
Revenue cycle leadership cannot manage what it cannot see. The quality and timeliness of reporting determines whether performance issues are caught early, when correction is cheap, or late, when revenue has already been lost and recovery is expensive.
Where traditional RCM Vendor excels?
Periodic reporting with retrospective performance views remains the standard in traditional RCM operations, and in stable environments with predictable payer behavior, retrospective data is often sufficient for effective management. Experienced account teams can contextualize reporting in ways automated dashboards cannot.
Where AI-powered Vendor excels?
Real-time dashboards with predictive and forward-looking insights allow leadership to act on trends before they become problems. When payer behavior shifts or denial patterns emerge, AI platforms surface the signal faster than any reporting cycle built around weekly or monthly reviews.
Note: Ask vendors to show you an actual reporting view from a current client with a similar revenue profile. The gap between what vendors describe in sales conversations and what they deliver operationally is most visible in reporting, and prospective clients rarely ask to see it before signing.
Integration and Technology Architecture
AI-powered platforms are only as effective as the data they receive. Integration complexity is consistently underestimated, and integration failures are one of the most common reasons implementations stall.
Where a traditional vendor excels?
The integration footprint for traditional RCM vendors is typically lighter, with fewer dependencies on real-time data exchange and more tolerance for manual coordination at handoff points. This reduces implementation risk, particularly for organizations with older or less flexible practice management systems.
Where AI-powered Vendor excels?
Deep system integration enables seamless data flow across workflows, connecting scheduling, eligibility, coding, claims, and denial management in ways that siloed architectures cannot. When integration is executed well, the downstream benefits compound across every stage of the cycle.
Note: Ask every vendor to walk through exactly how they would connect with your current systems before you reach the contracting stage. Evaluate API flexibility, data latency, uptime guarantees, and disaster recovery capabilities. If integration requires constant IT intervention or creates workflow disruptions for billing teams, AI adoption will slow regardless of platform quality.
Performance Metrics and Proven Outcomes
Promises mean little without evidence. Credible vendors anchor their proposals in measurable benchmarks and back them with documentation that can be independently verified.
Clean claim rates should be at or above 95 percent, with best-in-class performance reaching 98 percent or higher. Denial rates should be at or below five percent, national averages hover near 11.8 percent, so industry-average performance is not an achievement, it is a baseline. Days in A/R should trend below 30 for efficient operations. Net collection rates at or above 95 percent reflect genuine revenue capture.
Where traditional RCM Vendor excels?
Stronger metrics on complex recovery, higher appeal success rates, better resolution on aged A/R, reflect the value of human judgment and payer relationship capital in situations where automated platforms reach the limits of their rule sets.
Where AI-powered Vendor excels?
Stronger early metrics on prevention, fewer initial denials, faster clean claim rates, reflect the upstream impact of predictive analytics and continuous claim-level monitoring. Prevention performance compounds over time as the platform learns from your specific payer and coding environment.
- Ask for case studies from organizations that match your specialty mix and revenue profile.
- Ask for long-term performance data, not just post-implementation snapshots.
- Ask for specific examples of how vendors diagnosed and corrected underperforming revenue cycles, and which model, human or automated, drove the correction.
| Evaluation Criterion | AI-Enabled RCM Vendor Approach | Traditional RCM Vendor Approach |
|---|---|---|
| Revenue Performance Optimization | Uses predictive insights and automation to reduce revenue leakage and improve reimbursement outcomes | Focuses on improving collections through established workflows and historical performance |
| Operational Efficiency Model | Automates and intelligently allocates work to reduce manual effort and improve throughput | Relies on staff-driven execution and standardized manual processes |
| Risk, Denial & Compliance Management | Proactively identifies risks using analytics and continuous monitoring | Reactively manages denials and compliance through resolution-based workflows |
| Technology & Intelligence Capability | Leverages AI/ML, predictive analytics, and real-time decision support | Uses rule-based systems with limited automation and periodic analysis |
| Visibility & Decision Support | Provides real-time dashboards with predictive and forward-looking insights | Offers periodic reports with retrospective performance view |
| Scalability & Growth Readiness | Scales through automation and system intelligence with minimal manual effort | Scales through hiring, training, and expanding operational teams |
| Cost & Value Structure | Higher tech investment but improved efficiency and lower cost-to-collect over time | Labor-driven cost structure linked to staffing and operational volume |
| Integration & Ecosystem Alignment | Deep system integration enabling seamless data flow across workflows | Standard integrations with higher dependency on manual coordination |
| Organizational Fit & Strategy | Best for organizations seeking transformation, scalability, and data-driven optimization | Best for organizations prioritizing stability, consistency, and operational control |
Red Flags in RCM Vendor Evaluation
AI language without operational specificity
Ask how their models work, what data trains them, how frequently they update, and what happens when they underperform. Vague answers mean the AI is a marketing layer, not operational infrastructure.
Expertise claims without documented outcomes
Traditional vendors who rely on credentials and tenure without verifiable performance data are the mirror image of AI vendors with impressive demos and no proof of production results.
Case studies that do not match your profile
References from large health systems mean little if your organization runs $15 million across three specialties. If comparable evidence is absent, that absence is the answer.
Integration promises without specificity
For AI-powered vendors especially, ask exactly which EHR system versions they integrate with, how they have handled integration failures in previous implementations, and what the contingency is if data pipelines are disrupted.
Pricing that obscures total cost
AI-powered vendors commonly have hidden integration costs, model training fees, and onboarding charges not reflected in the headline rate. Traditional vendors often carry volume minimums and per-action billing. Every cost component should be documented before signing.
No willingness to tie compensation to outcomes
Vendors confident in their results, whether from a proven platform or experienced staff, will structure at least some compensation around measurable performance. Resistance to that conversation is itself a signal.
The RCM Operating Model Decision: What Works for Your Organization
An AI-powered RCM partner tends to deliver the strongest results when an organization has sufficient claim volume to train and benefit from predictive models, complex denial patterns that benefit from pattern recognition at scale, multi-specialty or multi-location complexity that strains manual tracking, and the operational readiness to absorb a technology-led transition.
It is especially well-suited for organizations with aggressive growth plans, payer mixes with high prior authorization volume, and leadership that wants real-time revenue intelligence rather than monthly summaries.
A traditional RCM partner may serve organizations better when human expertise, payer relationship depth, and appeals judgment are the primary value drivers.
Smaller single-specialty practices, organizations with stable payer relationships and lower denial complexity, and care providers whose primary RCM challenge is documentation quality rather than volume management may find that experienced human teams deliver more practical value than predictive automation.
The most effective model in many organizations is a hybrid: intelligent automation and AI dashboards handling the volume, pattern recognition, and reporting layer, with experienced human specialists focused on the decisions, escalations, and payer relationships where judgment matters most.
The Hybrid RCM Model That Most High-Performing Organizations Choose in 2026
The conversation around revenue cycle management is often framed as a choice between traditional human expertise and AI-driven automation. In practice, the most financially stable and operationally resilient organizations are not choosing one or the other.
They are combining both. The hybrid RCM model integrates intelligent automation and predictive analytics with experienced revenue cycle specialists who manage exceptions, payer escalation, and clinical documentation complexity.
Instead of replacing people with technology, the hybrid approach assigns each task to the capability best suited to handle it.
- Automation handles the volume.
- People handle the judgment.
- Leadership gets the visibility to manage both.
This hybrid RCM model reflects a simple financial reality: not every revenue cycle task benefits equally from automation, and not every denial can be resolved through software logic alone.
Organizations adopting hybrid RCM models typically see measurable improvements in both efficiency and revenue protection because they optimize the full cycle rather than focusing on a single capability.
Financial Impact of a Hybrid RCM Model
The value of a hybrid approach becomes most visible in the metrics that directly affect cash flow and operating margin.
Organizations transitioning from traditional or fully manual workflows to hybrid RCM structures commonly experience:
- 15 to 25% reduction in denial volume through predictive claim validation
- 10 to 20% faster payment cycles due to automated workflow prioritization
- 20 – 40% lower administrative cost growth during expansion
- Improved net collection rates through stronger prevention and recovery alignment
These improvements compound over time because prevention reduces rework, and automation reduces labor dependency.
The result is not just operational efficiency. It is financial stability.
Know your revenue cycle performance before selecting your next RCM partner.
Request a Performance Assessment from BillingParadise.
Ready To Build Revenue Resilience With the Right RCM Partner in 2026?
The comparison between AI-powered and traditional RCM services does not resolve to a universal answer. It resolves to the right answer for your organization’s specific profile, your claim volume, payer mix, technology infrastructure, denial patterns, credentialing complexity, patient intake workflows, and capacity to absorb change.
What does not change, regardless of the model you choose, is the standard worth holding.
A strong RCM partner, whether powered by intelligent automation or human expertise, protects revenue at every stage of the cycle, brings transparency to decisions that affect your organization’s financial future, and grows alongside you in a way that feels less like a vendor relationship and more like a shared stake in the outcome.
At BillingParadise, we have spent years building that kind of partnership with healthcare organizations, combining the depth of experienced RCM specialists with the efficiency of intelligent automation, AI-driven analytics, and modern EHR integration.
Whether you are evaluating AI-powered RCM services for the first time or reassessing a vendor relationship that has stopped delivering, we are here to help you approach that evaluation honestly.
When you are ready for a deeper conversation about what your organization specifically needs, we are here for that.








